There are many varieties of hormonal birth control available. Long before “the pill,” prevention of pregnancy was a hot button topic and continues to be so today.
In our modern world, birth control is prescribed for more than contraceptive use. Women who experience the following issues may also receive a prescription for birth control:
- severe menstrual cycles or chronic acne
- a history of endometriosis (excessive growth of uterine tissue)
- a diagnosis of polycystic ovarian syndrome (a disorder that causes cyst growth on the ovaries, unusual hair growth, severe acne, and disrupts menstrual cycles)
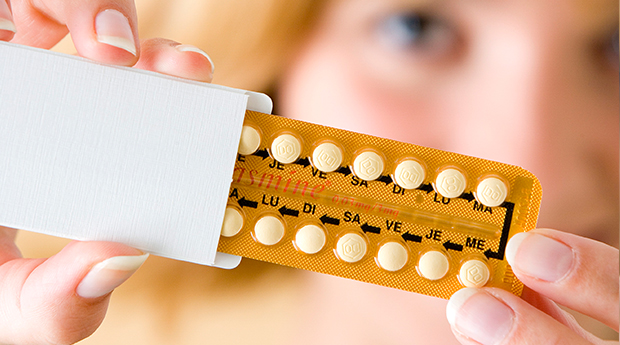
Hormonal birth control that is delivered via a pill, injection, patch, or delayed release mechanism (usually implanted beneath the skin) is currently the subject of an intense debate. While your choice of birth control is an intensely personal choice, it is important to know all the facts.
Hormonal Birth Control and Cancer: Is There a Connection?
The messages within the health community are decidedly mixed.
While pro-hormonal contraceptive experts have stated that birth control “lowers cancer risk” – there is a caveat. It has been proven that while these pharmaceutical versions may lower ovarian cancer risk, they raise your risk of liver, breast, and gynecologic (cervical, uterine, ovarian, vaginal, and vulvar) cancers overall.
There are two forms of hormonal birth control: progestin-only and combination: progestin-only pills contain the synthetic version of the progesterone hormone, and combination pills contain synthesized progesterone and estrogen. Hormonal contraceptives are made from artificial hormone-like substances that attempt to mimic the effects of naturally occurring hormones in the body. Synthetic progesterone and estrogens have been linked to a greater risk of breast and other cancers.
The Research on Hormonal Birth Control
In 2005, the World Health Organization (WHO) reported that “estrogen-progestin oral contraceptives” (combination pills) could cause cervical, liver, and breast cancer.
Researchers have found that progesterone and estrogen, two naturally occurring female hormones, affect the growth of some types of cancer cells. Since birth control pills contain female hormones, scientists are investigating the plausible links between cancer and oral contraceptives. However, it is important to understand that naturally occurring progesterone is cancer-preventive. Only the synthetic versions are an issue. Naturally occurring estrogens can be preventive or problematic, but the latter is only the case when there is insufficient progesterone.
There are several contributing factors for the development of breast cancer, which include a woman’s natural reproductive hormones. Some factors could increase the risk of cancer, such as exposure of the breast tissues to the estrogen hormones for longer periods of time. During specific stages in a woman’s life, reproductive hormones change in intensity. These factors seem to influence the development of breast cancer.
For example, women who started menstruating at an early age or entered menopause at a later age had longer exposure to estrogen. According to Mayo Clinic’s medical journal, women who took hormonal birth control before their first pregnancy have a higher risk of contracting breast cancer. Women using the Pill after the age of 45 have seen a 144% greater risk of developing breast cancer than women who have never used it.
Over 50 studies gathered by the Collaborative Group on Hormonal Factors in Breast Cancer indicated that women using contraceptive pills are more susceptible to breast cancer than women who don’t take contraceptives. Research published in 2011 in the journal Cancer Research significantly linked breast cancer to taking the pill. Logically they found that the high dose estrogen pills resulted in greater risk than lose-dose, but regardless, both increased the risk of breast cancer.
In The Breast Cancer Prevention Program, Sam Epstein, MD, writes, “more than 20 well-controlled studies have demonstrated the clear risk of premenopausal breast cancer with the use of oral contraceptives. These estimates indicate that a young woman who uses oral contraceptives has up to ten times the risk for developing breast cancer as does a non-user, particularly if she uses the Pill during her teens or early twenties; if she uses the Pill for two years or more; if she uses the Pill before her first full-term pregnancy; if she has a family history of breast cancer.”
One study showed that if you stop using hormonal birth control for 10 years or more, your body reverts to the state prior to the birth control, as if it was never used. Conversely, Iranian research in 2011 showed that the longer the women were on the pill, the greater the risk for breast and cervical cancer. They found that the use of oral contraceptives can double the incidence of breast cancer and triple the risk for cervical cancer. Importantly, however, they found no significant relationship between the age at discontinuation, patterns of use and intervals from last use with respect to risk reduction.
At the end of the day, any benefits a woman might gain from taking the pill are greatly diminished by the risks to her health.
Choosing Your Contraceptives
It is essential to monitor your health at all times and in all aspects of your life, including in the choice of your contraceptives.
Cancer isn’t the only health risk of hormonal birth control. These contraceptive methods have also been linked to other health issues such as high blood pressure, heart attack, stroke, and blood clots. In fact, one study found that women who use low-dose oral contraceptive pills have a two-fold increased risk of a fatal heart attack compared to non-users. Women over the age of 35 who smoke are usually not prescribed hormonal birth control due to increased stroke risk.
There are non-hormonal options available for women who’d rather not take the risk of putting excess hormones into their bodies. These options are for those who use birth control solely for pregnancy prevention and include the intrauterine contraceptive devices (IUD), the contraceptive sponge, Lea’s Shield contraceptives, calendar-based methods, condoms, cervical caps, diaphragms, as well as permanent options such as tubal ligation.
The right contraceptive for you is the one that works best with your lifestyle and level of health. Talk with your healthcare provider about the pros and cons of hormonal and non-hormonal forms of birth control so that you can make an informed decision.
Want to stay abreast of new ways to stay healthy? Be notified each week when cutting-edge articles are added by clicking here. You’ll be glad you did.
Article Summary
Hormonal birth control that is delivered via a pill, injection, patch, or delayed release mechanism is currently the subject of an intense debate.
Synthetic progesterone and estrogens have been linked to a greater risk of breast and other cancers.
It is important to understand that naturally occurring progesterone is cancer-preventive; synthetic versions are an issue.
Women who took hormonal birth control before their first pregnancy have a higher risk of contracting breast cancer.
These contraceptive methods have also been linked to other health issues such as high blood pressure, heart attack, stroke, and blood clots.
There are non-hormonal options available for women who’d rather not take the risk of putting excess hormones into their bodies.



















The most safest immoral way of using birth control is abstinence and working with your husband and the Lord on spacing your children out and abstinence so it’s pretty much Chastity within marriage where instant gratification Society so abstinence and Chastity is not talked about or used very much but it helps the marital couple grow in the Lord and grow closer together and keep Communication open marriage is actually for the state of children if one doesn’t want to have children when should not be getting married and one should be open to life at all times and marriage and accept the children that God will bring them hormonal birth control actually causes early term abortions within the first few weeks of pregnancy so more babies are being aborted through hormonal contraception than actual abortion and these babies are not baptized and do not and will not see the beatific vision of God and will be in Abraham’s bizom busam due to not being baptized so it’s a serious issue and marriage is actually a Blessed Trinity the wife the husband and the Holy Ghost and marriages that practice for control do not accept God’s will for their marriage do not accept the Blessed Trinity and are at risk for getting a divorce God’s will is always the best will.
I was on birth control for 28 years and stopped using it against my doctor’s recommendation. I have been off of the pill for 3 years now and I am still struggling to balance my hormones. I wish I would have known better at the time.
We’re so sorry to hear this, Julie. 🙁
We’ll be sure to keep you in our prayers!
Have a small pain at my breast
Hi Agnes –
We appreciate you reaching out to us about this.
Unfortunately, we are unable to give any kind of medical advice. The best advice we can give you is to consult with one of the doctors we interviewed in the Global series.
Please note that we are not able to select an expert for you.
We’ve created a page with the experts’ contact info as it was available to us.
Here’s the link to the actual webpage:
http://thetruthaboutcancer.com/experts-info-sheet/
We do have one more resource you may be interested in. During our Live Event 2017 series, Dr. Patrick Quillin suggested contacting The Institute of Functional Medicine to locate a practitioner in your area.
If you are interested, here is the link to search for a Functional Medicine Practitioner in your area: https://www.ifm.org/find-a-practitioner/
Praying for the very best for you!
Vasectomy could be at least me tio ed as a drug free option for the team who are I volved.
These non Harmonal methods are Not safe either. Usually the content is good here but I am sorry suggestions in this article is no good.
My doctor give me 25.years hormone pills 💊 then I get Breast-cancer .
These hormonal pills should not be used because they could cause high estrogen. Many women have enough high estrogen. We do not need more.