Editor’s Note: This article first appeared in the Sept 2015 edition of TTAC’s Insiders member newsletter.
Before the discovery of antibiotics, people had very little choice when dealing with an infection. The only choice was basically to “wait and see” if the body could overcome it on its own. For infected body parts there was also the grim option of cutting off the affected body part for fear of dying. This was an especially difficult choice back then because surgeries were routinely performed without anesthesia! It was not until 1928 that the very first antibiotic was discovered and the treatment of infection changed dramatically.
It’s true that antibiotics can help the body overcome infections faster. The significant downside though is that they also kill friendly bacteria in the intestines while killing off infection-causing bacteria. Eighty percent of the immune system starts in the gut, so anything interfering with gut health can potentially lead to various health problems, including cancer.
Just because doctors routinely prescribe antibiotics does not mean you should routinely take them. The word antibiotic actually means “against life” or “anti body.” There are many other ways to treat infection and maintain a healthy immune system. How we treat infections (both local as in a cut or wound or systemic such as a cold or flu) is greatly influenced by how we believe disease starts in the body.
The Battle of Two Theories: Is Disease Caused by Germs or Are Germs Caused by Disease?
The conventional way of “thinking” about disease is due to a choice that was made in the middle of the last century. Two French scientists, Louis Pasteur and Antoine Bechamp, were the center of controversial assertions and research over the Germ Theory and the Cellular Theory of disease. Bechamp’s research proved most disease is generated in the body when it is out of balance or malnourished. His theories stood consistent with thousands of years of history.
Pasteur plagiarized the more prominent Bechamp’s research, and claimed he had “discovered” germs. Ultimately, Pasteur’s theories won and were adopted by the allopathic medical movement, which embraced the theory that germs cause disease and the only way to treat disease is with pharmaceutical drugs. The basic belief adopted was that there are thousands of germs outside the body just waiting to attack us.
Pasteur’s theories are revered by modern medicine and have been the premise behind profitable “treatments” in the form of drugs, vaccines, and surgeries formulated by the pharmaceutical companies.
Pasteur’s Germ Theory:
- Disease arises from outside the body.
- Disease can “strike” anyone anytime.
- Bacteria should be fought and guarded against.
Bechamp’s Cellular Theory:
- Disease arises from cells within the body.
- Disease happens in unhealthy conditions.
- In homeostasis, micro-organisms function to build tissue and assist the body.
Because most of Western society has adopted the Germ Theory, antibiotics are being routinely prescribed without taking into account the future damage they may cause. In addition, because modern medicine is driven by profit and how high a stock can go to please investors, natural and alternative methods to combat bacterial and viral infections are almost never recommended by a conventional doctor.
Antibiotics Routinely Given Early in Life

Giving antibiotics to an infant will forever alter their immune system. According to a study published this year in the Journal Cell Host Microbe, “Recent epidemiological data suggests an association between early antibiotic use and disease phenotypes in adulthood.”
Antibiotics are often prescribed for childhood ear infections, which could likely be viral and not bacterial. Several studies have shown that over 80% of ear infections clear on their own without an antibiotic. Sadly, most children never reach their first birthday before being prescribed at least one antibiotic.
A closer look at ingredients will reveal many different additives along with the antibiotic drug: artificial colorings (of which there could be many), sugars, artificial sweeteners, and preservatives. These toxic additives are unhealthy for anyone, but especially a young child whose immune system is maturing.
The American Academy of Pediatrics has revised their guidelines on treating ear infections due to adverse side effects of antibiotics. As many ear infections are caused by viruses as well, the standard protocol is to “watch and wait” and see if the ear infection clears on its own. Nevertheless, early antibiotic use could be setting our children up for disease and cancer down the road.
The Overuse of Antibiotics
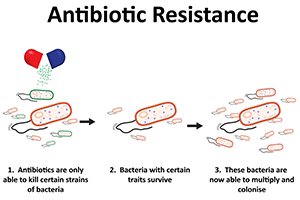
The US Centers for Disease Control recognizes that the overprescribing of antibiotics is contributing to a growth in antibiotic resistant strains of bacteria and creating a new set of problems for the public. Unfortunately, antibiotics aren’t just routinely given to humans; they are also present in our food supply. Most of the conventionally produced meats and dairy products (found in your typical grocery store, deli, and restaurant) contain antibiotics.
Since antibiotics don’t discriminate and also kill “good” bacteria in the gut, they can cause inflammation and destroy the immune system over time. Cancer is an inflammatory illness and antibiotics contribute to inflammation.
Antibiotic Use Linked to Cancer and Other Disease
Antibiotic use in childhood infancy (and any other time in life) is linked to various autoimmune diseases. Antibiotics cause imbalances in gut microbiota, called dysbiosis, which contributes to a weaker immune system. Weak immunity can potentially lead to a myriad of diseases and cancer.
The International Journal of Cancer published a study demonstrating the link between antibiotic usage and the risk for developing breast, lung, prostate, and colon cancer. The study also showed an increase in less common cancers such as cancers of the pancreas, bladder, kidney, and thyroid, as well as myeloma, leukemia, and non-melanoma skin cancers. Let’s look at how antibiotic use could have an effect on breast cancer and colon cancer in particular.
Research Points to an Elevated Risk of Breast Cancer
An article published by Dr. Josh Axe, a clinical nutritionist, doctor of natural medicine, and one of the Global Quest docu-series experts, cautions on the many dangers of antibiotics. He discusses two major studies that discovered an association between antibiotic usage and breast cancer.
One study published in the Journal of the American Medical Association (JAMA) showed that any amount of antibiotic use potentially increases breast cancer risk in women. Antibiotics increase the risk for cancer through its effects on inflammation, immune function, and metabolism of estrogen and phytochemicals.
The National Cancer Institute’s Division of Cancer Control and Population Sciences states this study shows an association between antibiotic use and breast cancer, but does not necessarily prove cause and effect.
Another study in Finland showed similar results: women who took antibiotics had an elevated risk of breast cancer. In addition, researchers from the University of Athens reviewed a number of published studies and concluded antibiotic use is linked to a slightly higher risk of breast cancer. With research like this, one should be cautious about antibiotic usage.
Could Altering Gut Flora Contribute to Colon Cancer?
In June 2014, Fox News reported on the increase in colon cancer associated with antibiotic use, citing studies that found colorectal cancer patients have a microbiome in the gut that is altered, compared to healthy people. Tissue from colorectal tumors also showed lower bacterial diversity, along with higher levels of certain harmful bacteria, which has been linked to a higher risk of colorectal cancer.
In one study, researchers looked at medical records of more than 22,000 patients over a period of six years in the United Kingdom. Patients who had a family history of colorectal cancer were excluded and risk factors for colorectal cancer such as diabetes, smoking, obesity, and alcohol consumption were controlled in the study.
The study compared the amount of antibiotics taken by a group of approximately 86,000 healthy people to the amount of antibiotics the colorectal patients took at least six months prior to being diagnosed with cancer. Results showed that those who had taken antibiotics, “including penicillins, quinolones and metronidazole, were 8 to 11 percent more likely to develop colorectal cancer.”
Despite the cancer industry’s failure to acknowledge a connection between antibiotic use and cancer, there are sufficient studies to indicate caution when choosing to take an antibiotic. Most of us have taken antibiotics at some point in our lives. Strengthening immunity and implementing natural remedies in place of antibiotics can go a long way towards repairing the damage our bodies have suffered as a result. Let’s look at this next.
Ways to Naturally Strengthen Immunity and Reverse Antibiotic Damage
The old adage “What doesn’t kill you, makes you stronger” just might be true. Your body is capable of overcoming most infections without antibiotics. When the body overcomes an infection naturally it builds a stronger immune system, whereas antibiotics weaken your immunity over time.
Antibiotics may help kill bacteria, but they do not always eliminate all of it. Additionally, they do not discriminate between the bad bacteria and healthy bacteria. Good bacterial flora is critical for immune system function and killing it creates an imbalance which contributes to both re-infection and the risk of new infection. It’s important to only use antibiotics when absolutely necessary for a serious illness and to supplement with quality probiotics.

If you do get an infection, there are many natural alternatives that are not only antibacterial, but also antiviral, antifungal, and antiparasitic. In most cases these are much better alternatives to powerful antibiotics and they likely won’t disturb the normal, healthy flora in your gut – at least not to the extent that an antibiotic will.
Top Natural Remedies for Infection
Silver: Despite the fact the medical establishment has not fully embraced silver as treatment for infection, there are nearly three decades of solid medical research demonstrating its powerful antiviral properties. This safe, natural mineral comes in a variety of forms, including colloidal silver.
Recent clinical research proves silver so powerful that it stops HIV from infecting human cells. The key is getting silver in extremely small particles that are nanometers (nm) in size. (A nanometer is one billionth of a meter.)
In June 2005, a 10-page study was published in the well-respected journal Nanobiotechnology proving that introducing tiny nano-particles of silver in a test tube with the AIDS virus alongside human cells, kept the virus from infecting the human cells.
Silver can be taken under the tongue for colds, flu, or other infections (both viral and bacterial), placed on the skin for cuts or skin infections, or even placed in the ear for an ear infection.
Silver comes in parts per million or ppm. More ppm is not necessarily better. In fact, I recommend only getting as high as 10 ppm while making sure the silver are nano-sized particles. Silver or nano-silver can be purchased in health food stores or online.
Garlic: Modern medicine is slowly beginning to recognize the amazing healing powers of garlic as antibiotics continue to lose their punch against superbugs such as MRSA. Garlic has been shown to help everything from the common cold to cancer, and more recently has been clinically shown to slow the growth of antibiotic resistant strains of bacteria, without disturbing normal flora.
One study showed a dramatic decrease in colds (64%) when supplementing daily with garlic and symptom duration was reduced by 70%.
Garlic has powerful antiviral, antibacterial, and antiparasitic properties, and is super easy to include in your daily meal plan.

Chopping garlic and allowing it to “sit” allows for more allicin (the compound in garlic containing antiviral and antibacterial properties) to be produced. You can add garlic to any dish for an immune boost such as steamed vegetables, guacamole, butter, mashed potatoes, soup, hot sauce, or even tea.
Oil of Oregano: Oregano may just be the most powerful of all natural antibiotics. There are over 800 studies demonstrating the power of carvacrol, a healing compound found in oregano. Carvacrol has been clinically proven by scientific research to reverse or decrease all of the following: viruses, parasites, infections (both bacterial and fungal), allergies, inflammation, tumors, E. Coli, and Candida.
Oil of oregano is extremely potent and it usually comes diluted with olive oil. The higher the carvacrol percentage, usually the more potent the oil. However, some companies will standardize to a high carvacrol percentage, but then add more carrier oil. If you are using straight essential oil of oregano, then it should be diluted with either water or oil (eg. olive or coconut oil). Dr. Axe recommends taking oil of oregano for up to two weeks maximum.
Dried oregano spice is fine for pregnant mothers, but pregnant women should use caution with oregano oil and only take as instructed by a qualified medical practitioner.

The following dosages of Echinacea have been scientifically studied for treatment of upper respiratory infections, including colds and flu:
- Echinacea liquid (Echinagard): 20 drops every 2 hours for the first day of symptoms, then 3 times daily for up to 10 days.
- A tablet containing 100 mg of a proprietary Echinacea angustifolia root extract (Monoselect Echinacea, PharmExtracta, Italy): 2 tablets daily for 15 days, then 1 tablet daily for 15 days, then 1 tablet every other day for 60 days to help prevent colds and the flu.
- Echinacea purpurea liquid: 0.9 ml 3 times daily for 4 months to help prevent colds.

A promising study in The Asian Pacific Journal of Tropical Biomedicine looked at the different types of honey and their effectiveness for anti-microbial resistant strains of bacteria, particularly for wound care such as burns. Tualang honey and Manuka honey were found to have powerful antibacterial properties against resistant strains of pathogens.
Furthermore, the study showed the benefits of locally produced honey compared to commercial brands. Honey is best if it’s local, raw, and unpasteurized.
Other natural remedies that can possibly be used in place of potentially harmful antibiotics include: olive leaf, astragalus, grapefruit seed extract, raw apple cider vinegar, virgin coconut oil, fermented foods, and supplemental probiotics.
From this list there is one particular remedy that I have found great results with. It is a remedy called Fire Cider. Fire Cider typically contains the following ingredients: raw apple cider vinegar, raw honey, fresh ginger, horseradish, onion, garlic, turmeric, cayenne, and sea salt. Search for recipes online on how to make this powerful cold and flu fighter.
Probiotics: The “Opposite” of Antibiotics
The prefix “pro” means “for” and “bio” means “life.” Probiotics help regenerate and populate the healthy or good bacterial flora in your small and large intestine. In the last decade alone, there have been over 5,000 published studies on probiotics in medical literature. Probiotics have been safely used for centuries all over the world, contributing to digestive health, and thus healthier immune function.
According to The World Health Organization, probiotics confer a health benefit to the body. Many common single-organism and composite probiotics in use today have been studied for efficacy.
As stated above, fermented foods contain probiotic bacteria and are an important inclusion into your diet. But finding a good probiotic supplement is also important, especially while taking antibiotics.
Seek out a probiotic with this highly effective strain – Lactobacillus acidophilus DDS-1. This strain has been shown in studies to colonize well in the gut.
It should be noted here that prebiotics are also important as they stimulate growth of healthy bacteria in the GI tract, which also promotes good health. Prebiotics are carbohydrates that are not digested by the body and provide a food source for the probiotics. Good sources of prebiotics include bananas, leeks, asparagus, garlic, onions, tomatoes, and other plants.
The Silver-Aloe-Probiotic Protocol
Dr. Robert Scott Bell, radio host and expert natural healer, developed this Silver Aloe protocol to rebuild gut integrity and treat chronic gut dysbiosis issues. The protocol uses silver hydrosel (Sovereign Silver), a high quality aloe vera juice (e.g. Stockton Aloe 1), and an intensive probiotic regimen.

Remember, with the majority of infections a healthy body knows how to respond. For most infections, one to two weeks of just waiting and doing nothing (except getting high quality nutrition and good sleep, of course) will do the trick.
In other cases you can likely shorten (considerably) the duration of most infections, by supplementing with natural remedies during that time. A good rule of thumb is to use a natural substance for as long as you would take an antibiotic (often 7 to 14 days).
Working with your body, instead of rushing to the doctor for a dose of gut and immune destroying antibiotics, can go a long way toward ensuring your overall good health and aiding in your prevention of cancer.
Article Summary
Most disease is generated in the body when it is out of balance or malnourished.
Antibiotics are being routinely prescribed without taking into account the future damage they may cause.
The over-prescribing of antibiotics is contributing to a growth in antibiotic resistant strains of bacteria and creating a new set of problems.
Antibiotics increase the risk for cancer through its effects on inflammation, immune function, and metabolism of estrogen and phytochemicals.
When the body overcomes an infection naturally, it builds a stronger immune system, whereas antibiotics weaken your immunity over time.
Probiotics can be a safer and more effective tool to boost immune function.




















I had a.full hip replacement 4 years ago and was just recently okayed to stop antibiotics before dental work. I now need to have a tooth pulled for having it replace with an implant. What is my best option for trying to prevent infection> I have organix oregano oil. Thank you for any help you can give me.
God Bless,
Sue
This is a highly informative article, I’m going to share it with all my friends and family.
Thank You! Valuable information. May you continue to prosper and be in good health even as your soul prospers.
I hold much praise for your dedication to a healthy life for all. Thank you so much for your contribution to mankind, keep up the good work Ty.
J D Wheeler.
Jerry,
Thank you for being part of our mission and reading our articles!
Is this guy adding colloidal silver to juiced aloe? There is a guy that sells the machine to add colloidal silver to your distilled water. Its this guy adding it to the aloe instead of water? Same concept?
My brother died from pancreatic tail adenocarcinoma (primary cause was cachexia). I will always know etiology of was prophylactic Clindamycin induced clostridium difficile infection. My father died from rare postcricoid hypopharyngeal tumor (primary cause was cachexia).as the result of sacral decubitus (MRSA/Strep B/antibiotics) with open sinus tract. Conventional medicine & Big Pharma falsify death certificates to profit and cover up iatrogenic disease.
Antibiotics should never be used except in dire circumstances because they kill the bad bacteria and the good bacteria too. Your gut is like a first and when you cut all the trees down in a forest it takes time for them to fully grow back. This is the same for good gut bacteria as explained by Dr. Steven Gundry. Once wiped out by antibiotics the good bacteria in the gut takes a very long time to reconstruct itself and allows us to be in healthier faster again.
The solution it a prebiotic and to enhance the effectiveness of a probiotic I use a probiotic. So take both. Anything we can get directly from food is always healthier than a man made version of it, however I suggest getting these the best way possible. ( Dr. Gundry created a prebiotic powder that I take daily along with a probiotic and several other things such as turmeric, cinnamon, echanica and many other supplements).
Another friend of mine named Bryan Johnson has a very important slogan for his health business and it’s very true and we should all heed his advice. “If you don’t make time for your WELLNESS….. you WILL make time for your illness”.
So everyone please
1) cut out or back on sugar
2) get an alkaline body by increasing your pH level
3) consume things with a high frequency ( I’m currently writing a cutting edge book on this info)
4) cut out processed foods and foods that cause inflammation.
5) eat berries daily and fruits and veggies and less meat
6) get enough rest and sleep
7) keep you body frequency up by thinking happy positive thoughts and LAUGHING out loud daily. Watch comedies and no horror films. Our thoughts affect our bodies on a cellular level.
8) have good gut health. Did you know that the bacteria in your gut actually can communicate with each other AND your brain? When you want a cookie it is your bacteria in your gut sending signals to the brain that it wants a cookie not an orange so take a prebiotic and a probiotic to the good bacteria outnumber the bad and you have good gut health and stay healthy.
9. Take supplements that you need to stay your healthiest.
10. Get direct sunlight everyday and walk barefoot on the grass to ground your body and accept the Earth’s healing.
11 Get human touch everyday. When we hug someone 20 seconds we create healing in both bodies. Also close contact with a pet increases our immunity.
12) FEEL UNCONDITIONAL LOVE for all life everywhere as this is our true path to human enlightenment and love has the highest frequency of all !
Peace – Love and wellness to all!
love the articles… all the TRUTH there is about health… m glad someone is trying to hammer some sense in to the mad world running after the mirage of western medicine. all you recommend synchs with all I have grown up to practice and believe and experience as true while I grew up and still live in India among the tit bits of ancient Yurveda and Yoga.
keep up the good work !
My last antibiotic use was back in the 80 because of a nasty cough that won’t go away no matter what for almost two months. Tetracycline was prescribed and I was down and out for almost two weeks after the dosage. I cannot take antibiotic or Vicodine without suffering more because of the drugs.
I am now only using herbal or homeopathic remedies. It works a lot better on the body.
Great to hear that homeopathic remedies have worked so well for you Karen!
Thank you, very informative, I wish I knew all this information 4 years ago when I had bad stomach bug Gardia and 10 years prior H B Piloris. I was given strong antibiotics for both..
I will only be using herbal. remedies from now on.
How I wish I had this information in 2013 when diagnosed with Prostate cancer. Allowed myself to enter into 7 weeks of daily Radiology, hormone jabs, suffocating sweating, poor sleep (constant trips to the toilet) virtually incontinent, and very worried.
5 years after the ‘All Clear’ much of the above side effects continue, plus a couple more.
Now a confirmed active follower of the ‘Truth about Cancer’ to ensure no return to a high PSA count.
My beloved dog Smokey died recently of Leukemia, and he was only 8 1/2. Vet kept him on way too much antibiotics, Baytril for long term off and on. And gave no probiotics to counter. He was on Baytril for reoccurring prostate infection. So, very reluctantly I agreed to neutering him. Just 2 weeks after neutering, he became very sick; vomiting up everything he ate and then stopped eating for several days. He was then quickly diagnosed with Acute Leukemia and became anemic. I’m guessing the irresponsible over use of antibiotics brought on Leukemia and Anemia by killing off his red blood cells. He never recovered but I wish I had waited longer for him to possibly recover. On his final day, Smokey’s face had swollen from taking steroids. If he had never been put on antibiotics to the extent he was, and then operated on, even though it was noticed he lost noticeable weight on surgery day, my strong belief is he’d never have contracted Leukemia and he’d still be alive today. But I put trust in vets who basically killed my dog, my Shepherd-Boxer Smokey. If I had only known the damage these strong antibiotics were doing to destroy his gut and thus the entire breakdown of his immune system. I’m just as guilty as them, but them moreso; they are the professionals who should have known better. Smokey died needlessly this past February 11, 2019, in Mississauga, Canada. The clinic I hold responsible: South Peel Animal Hospital; Dr Bob Smith and Dr Grace Jutras, who went ahead operating on Smokey even though she acknowledged he had lost weight. RIP Smokey. I am so sorry for what I did to you. Please forgive me. I will never forget you and will forever love you! – Shane McNeil
Hi Shane –
We’re so so sorry to hear about your loss.
Losing a pet is no different than losing a member of your family. This must have been beyond devastating.
I’m sure that Smokey must have known your love was genuine and that you did your absolute best for him.
Thank you for sharing this with us.
Wishing you endless love and comfort.
England boss Gareth Southgate started Lingard, 24, in his first two World Cup qualifiers and also played him in the draw against Spain in a friendly.
Adding honey to your drinks can help soothe sore throats